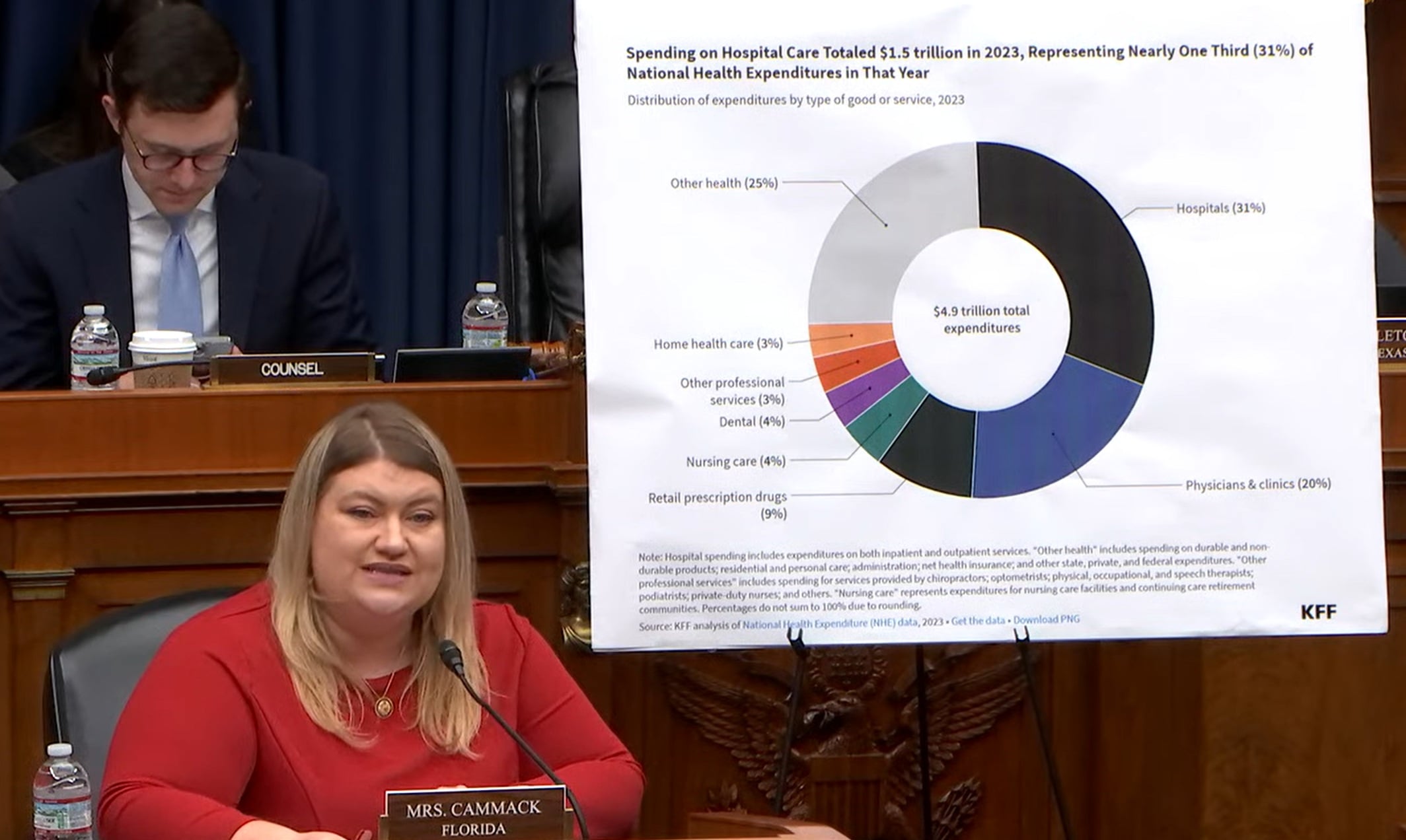
Provider consolidation was tip of the tongue Wednesday during a hearing that sat hospital and physician association leaders across from legislators.
Members of the House Energy and Commerce Committee’s Subcommittee on Health often returned to the issue when seeking answers on the drivers of, and solutions for, Americans’ rising healthcare costs.
Other policy issues including physician reimbursement, price transparency and the 340B drug discount program curbs also received airtime and legislator support—primarily from the subcommittee’s Republicans, as Democrats nearly to a man sought to underscore what they described as the more existential threats to access as well as affordability stemming from the One Big, Beautiful Bill Act’s sweeping Medicaid cuts.
Witnesses who testified were largely agreeable with the questions and suggestions from each side of the aisle.
For instance, speakers from the American Medical Association (AMA), the American Academy of Family Physicians (AAFP) and the Purchaser Business Group on Health (PBGH, the outlier among a provider-dominated panel) each affirmed that increasing government reimbursement for physicians would help practices remain independent. That could stem the tide of practice acquisitions by health systems, payers and private equity that most witnesses—and lawmakers—agreed have pushed prices upward.
“The physicians in America are in crisis in terms of reimbursement and payment,” David H. Aizuss, M.D., chair of the AMA Board of Trustees, told Rep. Neal Dunn, M.D., R-Florida, during the hearing. “Costs are rising dramatically, whether it’s the cost of insurance, the cost of rent, the cost of employees—the cost of everything we do to maintain our practices as a business and keep them open. That crisis is what’s accelerating further consolidation, and independent practices to go out of business. So, anything that would prevent that from occurring would be beneficial.”
Under current statute, physician payments are scheduled to decline in the coming year alongside the expiration of a one-year pay bump. For a solution, Aizuss, AAFP CEO R. Shawn Martin and Anthony DiGiorgio, D.O., a neurosurgeon at the University of California San Francisco Health and a health policy researcher affiliated with the Mercatus Center, each pointed to a prior call from the Medicare Payment Advisory Commission (MedPAC) to tie physician payment updates to the Medicare Economic Index (MEI), which measures practice cost inflation.
Elizabeth Mitchell, president and CEO of PBGH, said the self-insured employers who make up the group’s membership would have no problem paying the subsequent higher rates to independent doctors.
“Our members want to pay more for independent physicians because we know that it leads to better referrals, based on quality, it leads to lower costs, and the distortion of pricing in hospitals is highly problematic,” she said referring to hospital facility fees and site-of-service payment differences.
Playing on-and-off defense through the hearing was Rick Pollack, president and CEO of the American Hospital Association (AHA).
On acquisitions of practices, he told Dunn the hospital sector has become less of a driving force in the last four years compared to private equity, medical groups and insurers, in that order. He added that physician employment isn’t the only way for hospitals and doctors to affiliate, “but sometimes we are approached by physicians who want to be part of a hospital system.”
Other lawmakers often brought up potential repeal on the Affordable Care Act’s moratorium on the opening of new physician-owned hospitals, reform of anti-kickback rules on self-referrals DiGiorgio said more harshly target physician-owned entities than larger systems, and the implementation of site-neutral payment policies. Most of the panel signaled varying levels of support for such legislative changes, with Pollack, representing hospitals and health systems, again being the odd one out.
Some representatives polled the panel on whether large, and growing, health systems are beneficial to the system or another source of rising costs. Pollack looked to paint against the grain, citing data that operating costs for merging systems are reduced by an average of 3.3% alongside other decreases in revenue per adjusted admission and quality improvements.
“Now the issue, congresswoman, is that doesn’t always get passed on to the patient because there’s a patient in between that sets the rates,” he told Rep. Kat Cammack, R-Florida, while noting how some deals can save failing hospitals.
“I think the data points to a completely opposite scenario than what you just painted,” Cammack replied. DiGiorgio and Mitchell echoed her skepticism in their responses to questions, describing reduced competition and higher costs stemming from health systems’ outsized market control.
Some lawmakers specifically pointed to the witnesses’ responses toward recent headlines.
Rep. Michael Rulli, R-Ohio, outlined a lawsuit filed last month by the Department of Justice and the Ohio attorney general alleging OhioHealth has been using its scale to force payers into noncompetitive, all-or-nothing contracts. He asked whether such behavior was typical of large, competitively powerful hospitals, to which Mitchell said “we see that regularly across the country. When hospitals consolidate and you want access to any member of that system, it is harder to do that at a fair price when they are consolidated—and there have not been benefits in terms of better quality or access.”
Rep. Nanette Diaz Barragán, D-California, highlighted Sutter Health’s $575 million 2021 settlement over allegations of anti-competitive practices enabled by its scale, as well as the announcement earlier this week that it plans to absorb Allina Health. Pollack told her that the latter was of no anticompetitive concern because the California- and Minnesota-based systems operate in different markets.
Barragán was among the few Democrats during Wednesday’s hearing that did not devote their time to the impacts of the One Big, Beautiful Bill Act, which includes about $1 trillion of various Medicaid cuts and insurance enrollment hurdles over the course of a decade, or to Republicans’ recent decision not to extend enhanced subsidies for Affordable Care Act marketplace plans at the end of last year.
The minority party had witnesses voice the healthcare industry’s consensus predictions that the OBBBA, or H.R. 1, would lead to reduced coverage, higher premiums and an expected rise in poor outcomes and uncompensated care.
Rep. Raul Ruiz, M.D., D-California, likened Republicans’ questioning on policy tweaks to emergency department physicians debating a patient’s liver problems while ignoring the gunshot wound in their chest.
“[Patients] don’t give a s**t about consolidation right now when they’re sick,” Ruiz said. “They need healthcare now, and when they don’t get it … because they can’t afford their healthcare insurance, or they took it away because of the Medicaid cuts, they’re going to go where Mr. Pollack? The emergency department. That’s going to be uncompensated care for you.”
Financially strained hospitals facing increased uncompensated care will likely need to close low-margin services or entire facilities, Pollack confirmed at Ruiz’ prompting, as well as to renegotiate their contracts with payers. Payers will then increase premiums for employers and plan members, Ruiz said while referencing testimony recently given by insurance executives earlier this year.
“Suddenly everyone is paying more—that’s the gunshot wounds to the body coming into our emergency department that we need to take care of,” he said. “Let’s stabilize this patient by reversing these damages, and then let’s talk about consolidation, workforce problems and … tying reimbursement to MEI fully.”
Publisher: Source link