In 2024, almost all states completed renewals for the 94 million individuals who were enrolled in Medicaid following the pandemic-era three-year pause on disenrollments that was lifted on March 31, 2023. By October 2024, based on the most recent Centers for Medicare and Medicaid Services (CMS) enrollment data, the process known as unwinding had resulted in a net decline in Medicaid and CHIP enrollment of 15 million individuals, including about five million children, but enrollment remained above pre-pandemic levels.
The focus on Medicaid renewal processes during the unwinding revealed their complexity. With states facing an unprecedented volume of work and eligibility worker shortages, CMS provided new options to streamline enrollment and renewal processes, emphasizing automation and the use of reliable data sources to increase accuracy and efficiency. States broadly adopted these strategies, and many emerged from the unwinding with more efficient processes by maximizing the use of technology to verify income, reduce returned mail, and improve communications with enrollees. However, some states continue to struggle with older systems that limit the adoption and effectiveness of some of the new strategies.
Medicaid agencies are now turning their attention to ensuring that state policy aligns with existing and new federal requirements. At the same time, there is significant uncertainty about how potential changes to federal Medicaid financing and policy under consideration by Congress and the Administration will impact states and Medicaid enrollees in the future. Congress is debating cuts to Medicaid of up to $880 billion or more over ten years, citing a desire to curtail spending to help pay for tax cuts and address “fraud, waste, and abuse”. While several proposals would fundamentally restructure who is covered by the program and how it is financed, repeal of regulations finalized in the last administration, including the Eligibility & Enrollment (E&E) rule finalized in April 2024, are also under consideration. The E&E rule included provisions to streamline and enhance the administrative efficiency of Medicaid eligibility and enrollment processes and to make it easier for eligible individuals to retain coverage. The rule also clarified documentation and recordkeeping requirements, providing the first update to these requirements since 1986, to reduce payment errors based on insufficient documentation. By eliminating some barriers to enrollment and reducing churn among people who are eligible but lose coverage for paperwork reasons, the rule is expected to increase Medicaid and CHIP enrollment (CMS projected enrollment would increase by 1.5 million in 2028.) The Congressional Budget Office estimated that rescinding this rule along with a related rule that reduces barriers to enrollment among people eligible for Medicare Savings Plan (MSP) coverage would reduce federal Medicaid spending by $164 billion over ten years.
The 23rd annual survey of state Medicaid and CHIP program officials conducted by KFF and the Georgetown University Center for Children and Families provides a baseline of state Medicaid and CHIP eligibility, enrollment, and renewal policies in place as of January 2025 as states return to routine operations following the unwinding. The report focuses on policies for children, pregnant individuals, parents, and other non-elderly adults whose eligibility is based on Modified Adjusted Gross Income (MAGI) financial eligibility rules. Overall, 49 states and the District of Columbia responded to the survey, although response rates for specific questions varied (Florida did not respond). For the purposes of this report, the District of Columbia is counted as a state.
Key Takeaways
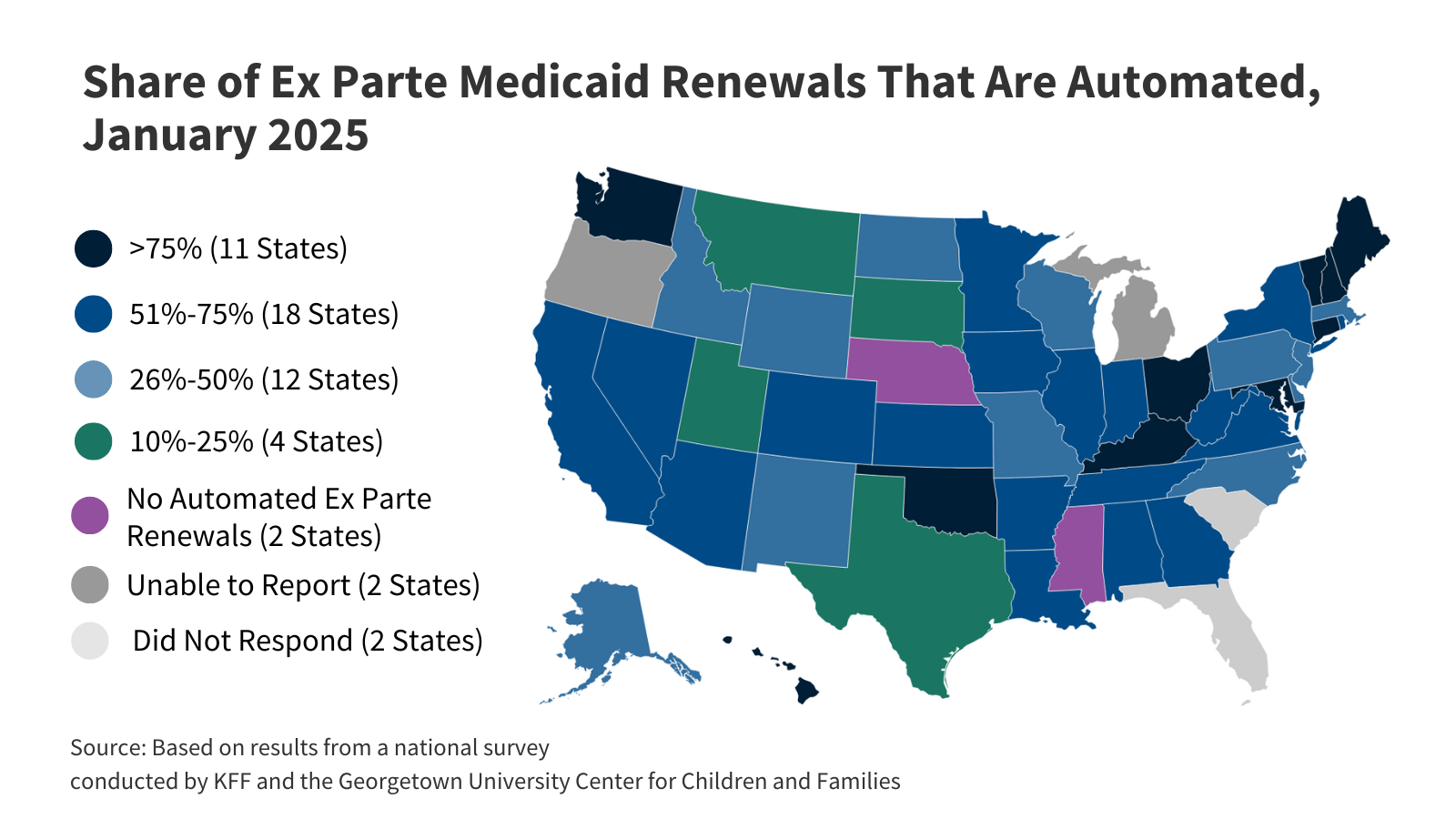
- Building on strategies adopted during the unwinding, most states are continuing to implement policies to increase ex parte, or administrative, renewal rates. During the unwinding period, states employed new approaches to using data and automation to streamline processes for verifying eligibility. Over two-thirds of states plan to continue or newly adopt at least one strategy to facilitate ex parte renewals. While 29 states report that over half of ex parte renewal rates are conducted automatically by their systems, the share of eligibility determinations at application that are automated and conducted in real-time (within 24 hours) lag. Close to half of states say they cannot conduct automated real-time eligibility determinations on new applications or report that less than 10% of these eligibility determinations are automated.
- States increasingly rely on data from trusted sources to automate manual tasks and improve accuracy of Medicaid eligibility, enrollment, and renewal processes. By advancing the use of information from other programs such as SNAP and TANF, states have improved the accuracy of income verification while reducing administrative burden associated with mailing renewal forms and manually processing information submitted by mail or phone. At the same time, periodic checks of income data sources coupled with limited time for enrollees to respond to information requests can increase procedural disenrollments and churn.
- States have incorporated new strategies for updating contact information and communicating with enrollees into routine operations, and some are using artificial intelligence (AI) to assist with the application and renewal processes. Access to the US Postal Service National Change of Address (NCOA) Database and other program data allows states to routinely update mailing addresses, tackling the longstanding problem of returned mail. Nearly all states proactively check available data sources for updated contact information or accept updated addresses from managed care plans or providers. To increase renewal response rates, states contact enrollees multiple times before and after sending renewal notices using multiple modes including email and text. States have also enhanced online tools–online accounts and mobile apps–to provide additional ways to communicate with enrollees and to give enrollees the ability to more easily manage their coverage. A few states use AI to answer consumer questions at different points during the application or renewal process, and a small number have begun using AI to assist with reviewing applications and renewals.
- Continuing a trend over the past few years, two states increased income eligibility for pregnancy coverage. Alaska and Washington state expanded income eligibility for pregnancy and Colorado adopted the From Conception to the End of Pregnancy coverage option in CHIP. Since 2023, five states (Alaska, Nevada, North Dakota, Tennessee, and Washington) have increased pregnancy eligibility levels, but one state (Iowa) is seeking approval to reduce pregnancy income eligibility. The median eligibility level for children (255%) is the highest of all MAGI groups. Eligibility levels for all MAGI groups are lower in non-expansion states compared to expansion states.
- States have taken steps to remove administrative barriers to enrollment and renewal for children and seniors and people with disabilities (non-MAGI groups). Almost all states with separate CHIP programs have eliminated required periods of uninsurance (waiting periods) and lock-out periods following nonpayment of premiums, both of which contribute to gaps in coverage. The E&E rule requires states to phase out waiting and lock-out periods by June 2025. Two states (Utah and Delaware) permanently eliminated CHIP premiums in 2024, and premiums remain temporarily or indefinitely suspended in Arizona and Vermont while Georgia reinstated CHIP premiums after pausing them during the COVID pandemic. All states have taken steps to align non-MAGI renewal rules with those in place for MAGI groups such as conducting annual renewals, eliminating in-person interviews, and giving enrollees more time than 10 days to respond to requests for information. The E&E rule requires states to align non-MAGI renewal policies by June 2027.
Publisher: Source link