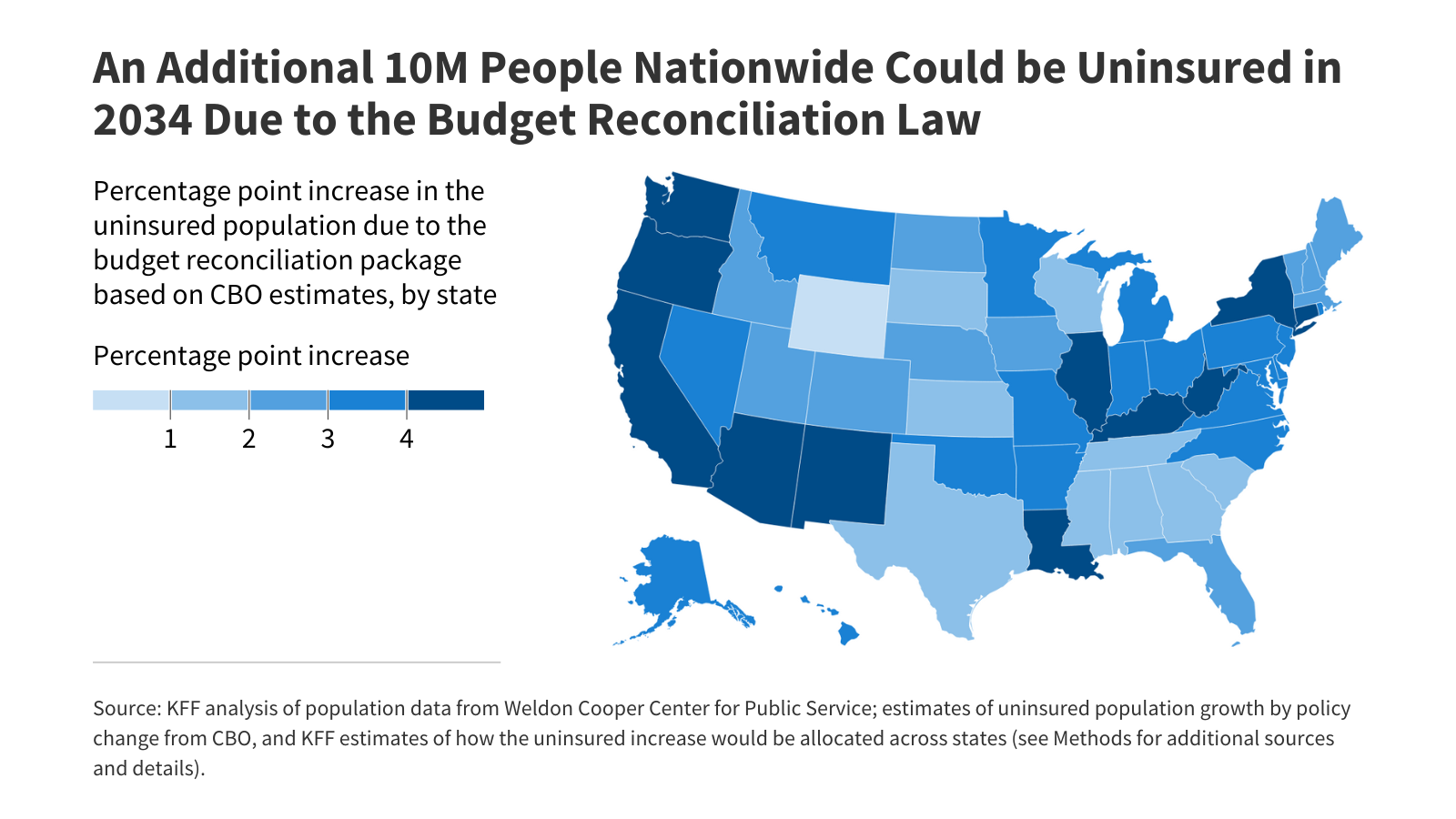
President Trump signed into law on July 4, 2025 a budget reconciliation package (formerly called the “One Big Beautiful Bill Act”) that will make significant changes to Medicaid and the Affordable Care Act (ACA) Marketplaces. The Congressional Budget Office (CBO) estimates that, relative to its estimates of insurance coverage prior to the law being enacted, the law will increase the number of people without health insurance in 2034 by 10 million, because of changes to Medicaid (7.5 million), the ACA Marketplaces (2.1 million), and other policies and interactions among different provisions (0.4 million). These legislative changes come at a time when enhanced premium tax credits for ACA Marketplace enrollees are set to expire later this year. When combining the impact of the reconciliation law with that of the expected expiration of the ACA’s enhanced premium tax credits, CBO estimates show that the number of uninsured people will increase by more than 14 million in 2034. That estimate does not account for the effects of the Trump administration’s ACA Marketplace Integrity and Affordability rule finalized earlier this year, so the overall change in the number of uninsured people could be even larger.
This analysis apportions the increase in the number of uninsured across the 50 states and the District of Columbia and shows that number as a percentage of each state’s population. The number of additional uninsured people as a percent of the population is equivalent to the percentage point increase in the 2034 uninsured rate. Nationally, CBO projected an uninsured rate of under 10% in 2034 under current law, which assumed the enhanced ACA premium tax credits would expire. The analysis here includes two maps: one showing the effects of the reconciliation law, and another showing those effects combined with expiration of the ACA enhanced premium tax credits. (The ACA Marketplace Integrity and Affordability rule is expected to contribute to increases in the uninsured, though estimates of the finalized rule have not been released by CBO.)
Anticipating how states will respond to changes in Medicaid policy is a major source of uncertainty in CBO’s cost estimates. Instead of making state-by-state predictions about policy responses, CBO estimates the percentage of the affected population that lives in states with different types of policy responses. For example, in the reconciliation law, Medicaid work requirements account for more than half of CBO’s estimated 2034 increase in the number of people without uninsurance because of changes to Medicaid. However, different states might choose to implement a work requirement with reporting requirements that are easier or harder for enrollees to comply with. Reflecting the uncertainty, this analysis illustrates the potential variation by showing a range of enrollment effects in each state, varying by plus or minus 25% from a midpoint estimate.
The interactive table at the end is sortable by state and size of increase in the uninsured rate.
Relative to current law, the reconciliation law is estimated to increase the uninsured rate by 3 percentage points or more in 20 states (Alaska, Arizona, Arkansas, California, Connecticut, Delaware, Illinois, Indiana, Kentucky, Louisiana, Montana, New Jersey, New Mexico, New York, Oklahoma, Oregon, Rhode Island, Virginia, Washington, West Virginia) and the District of Columbia. These increases are attributable to the reconciliation law alone and do not include the effects of the expiration of the enhanced premium tax credits or the proposed Marketplace integrity rule.
In terms of increases in the number of uninsured people, California and New York are the top two states (1.6M and 860k, respectively). Florida, Texas, and Illinois would follow at 590k, 480k, and 470k, respectively.
The combined effects of the budget law and the expiration of the ACA enhanced tax credits, compared to a scenario where the enhanced subsidies are in place, results in the greatest increases in Louisiana, Florida and Arizona, where the uninsured rate is expected to increase by at least 5 percentage points. In 34 states and the District of Columbia, the uninsured rates could be 3 percentage points or more higher than would otherwise be the case.
About half (49%) of the 14.2 million more people who would be uninsured in this scenario live in California (1.7M), Florida (1.5M), Texas (1.4M), New York (860k), Illinois (520k), Georgia (500k) and Ohio (460k). The largest growth in ACA Marketplace enrollment since 2020, the year before the enhanced premium tax credits became available, occurred in 3 of these states: Texas (2.8M), Florida (2.8M), and Georgia (1.0M).
Additional increases in the number of uninsured people in 2034 can also be attributable to the implementation of the finalized ACA Marketplace Integrity and Affordability rule. CBO has not released estimates for the finalized rule, so those effects are excluded from this analysis. In prior estimates, CBO allocated half of the 1.8 million increase in the uninsured due to the proposed Marketplace Integrity and Affordability rule to its baseline while they allocated the remainder into the Energy and Commerce section of the budget reconciliation bill. CMS estimates that in 2026, the finalized rule will lead to an increase in the number of uninsured people of between 725 thousand and 1.8 million. Many of the key provisions that impact enrollment processes will sunset at the end of 2026, so decreases in coverage from the rule in subsequent years are anticipated to be lower.
Methods
Increases in the number of uninsured were sourced from Congressional Budget Office (CBO) estimates, separated into three groups: those newly uninsured because of changes in Medicaid, those newly uninsured because of changes in the Affordable Care Act exchanges, and others.
Changes in Medicaid: CBO estimates that changes in Medicaid from the budget law are expected to decrease the number of people with health insurance by 7.5 million in 2034, relative to estimated coverage prior to the bill’s enactment. The CBO estimates show the uninsured increases provision by provision and KFF allocates each provision’s increase across the states proportionally to that provision’s estimated reduction in federal Medicaid spending from a prior KFF analysis. Additional details are in the prior analysis but in general, changes that would affect the ACA expansion group only, including work requirements, are allocated across expansion states proportionally to federal spending among people eligible for the ACA expansion in FY 2024. Provider tax provisions are allocated across the states using several steps that account for the different provider taxes states had in place prior to the bill’s enactment. Other provisions are allocated proportionally to states’ share of federal Medicaid spending in FY 2024. The sum of each provision’s increased in the number of uninsured people led to 8.0 million, which is more than the 7.5 million total, so each provision’s change was reduced by roughly 6% so that the provision-specific estimates would sum to 7.5 million. Data sources include:
Changes in the ACA Marketplaces: Increases in the uninsured population are taken from Congressional Budget Office estimates. Impacts of individual provisions within the budget reconciliation law are separately apportioned to calculate state-level estimates.
| Provision | Allocation Method | Source |
| Tax credit restrictions for immigrants | Share of noncitizens with direct-purchase health insurance | KFF analysis of 2023 American Community Survey (ACS) data |
| Eligibility verification requirements | Share of 2025 Marketplace enrollment | Open Enrollment Period Public Use Files |
| Prohibiting tax credit eligibility for non-qualifying life event SEP enrollees | Share of low-income enrollment (at or below 150% FPL) excluding the District of Columbia and states with Basic Health Programs or equivalent (MN, NY, OR) | Open Enrollment Period Public Use Files |
| Eliminating limits on excess premium tax credit repayments | Share of 2025 Marketplace enrollment | Open Enrollment Period Public Use Files |
Growth of the uninsured population due to the expiration of enhanced premium tax credits was allocated at the state level by share of growth in Marketplace enrollment between 2020 and 2025, based on the open enrollment period public use files. Due to rounding in the CBO estimates, increases in the uninsured due to individual provisions have been scaled to sum up to the totals provided by CBO.
Other Changes: The CBO estimates of changes in the number of uninsured people (relative to current law) include 0.1 million uninsured because of changes in Medicare and 0.3 million people uninsured because of interactions. Medicare-related changes are allocated proportionally to Medicare enrollment in 2024. Increases in the uninsured stemming from the interaction was split between Medicaid-related and ACA-related proportionally to each type’s chare of uninsured changes in CBO’s estimate (7.8 million for Medicaid and 2.1 million for ACA). Each change in the uninsured loss stemming from the interaction was allocated across states proportionally to each state’s share of the overall change.
Population Estimates: Decennial state-level population projections from the Weldon Cooper Center for Public Service are used to interpolate the population in 2034 assuming compound population growth. The percentage point increase of the uninsured population per state reflects the estimated increase in the uninsured as a share of the projected population. The total impact from all changes were aggregated then rounded to two significant figures, with the percentage point increase in the uninsured population rounded to the nearest whole number.
Publisher: Source link