Lawmakers in the U.S. House of Representatives proposed bipartisan legislation Monday aimed at strengthening Medicare Advantage plan oversight to ensure seniors receive timely and high-quality care.
Pennsylvania Republican John Joyce, M.D., introduced the Medicare Advantage Improvement Act of 2026 (PDF) on April 20. The bill aims to “directly address” barriers to coverage and treatment, according to an April 22 press release. The proposal would:
- Strengthen oversight and accountability for plans failing to meet compliance standards
- Increase transparency and streamline prior authorization processes to reduce care delays
- Align coverage criteria with traditional Medicare to ensure consistency
- Reduce administrative burdens through real-time, automated systems
- Expand access to post-acute care providers
“Medicare is a promise to America’s seniors that they will have dependable access to quality healthcare in their later years. However, that promise has been undermined by unnecessary barriers to care—particularly through excessive use of prior authorization and inappropriate coverage denials in Medicare Advantage,” Joyce said in a statement. “As a physician, I have seen firsthand how these delays harm patients and take valuable time away from the doctor-patient relationship. The Medicare Advantage Improvement Act will restore accountability, reduce unnecessary barriers, and ensure that seniors receive timely, high-quality care.”
The bill was co-sponsored by Reps. Kim Schrier, D-Wash., Gregory Murphy, R-N.C., Jimmy Panetta, D-Calif., Mariannette Miller-Meeks, R-Iowa, Ami Bera, D-Calif. And Beth Van Duyne, R-Texas.
“Health insurance companies have abused Medicare Advantage plans for too long, and they continue to skyrocket costs, deny coverage, and force taxpayers to pay the price. We need increased oversight into the Medicare Advantage program so that all seniors get the care they were promised,” Schrier said in a statement. “I am extremely proud to have worked on these much-needed Medicare Advantage reforms, which will hold insurance companies accountable and get patients timely, quality care.”
The American Health Care Association and National Center for Assisted Living (AHCA/NCAL) praised the legislation in an April 23 statement.
AHCA/NCAL President and CEO Clif Porter said the bill “represents a significant step towards ensuring Medicare Advantage delivers on its promise to America’s seniors.”
Moreover, AHCA/NCAL Vice President of Reimbursement Policy and Population Health Nisha Hammel said it “addresses many of the obstacles driven by insurer-led Medicare Advantage plans” that make navigating options and receiving coverage “unnecessarily difficult.”
“Coverage decisions for Medicare Advantage beneficiaries must be driven by each patient’s needs and clinical necessity, with appropriate oversight that ensures compliance and patient protections,” Hammel said.
St. Louis-based Ascension also announced its support for the legislation, with executives asserting that “too many patients face unnecessary delays, denials, and hurdles that interfere with timely and necessary care.”
Ascension President and CEO Eduardo Cornado said the system is “committed to being part of the solution.”
“This legislation is an important step toward strengthening the doctor-patient relationship, improving transparency, and helping Medicare Advantage better serve seniors and the clinicians who care for them,” Cornado said.
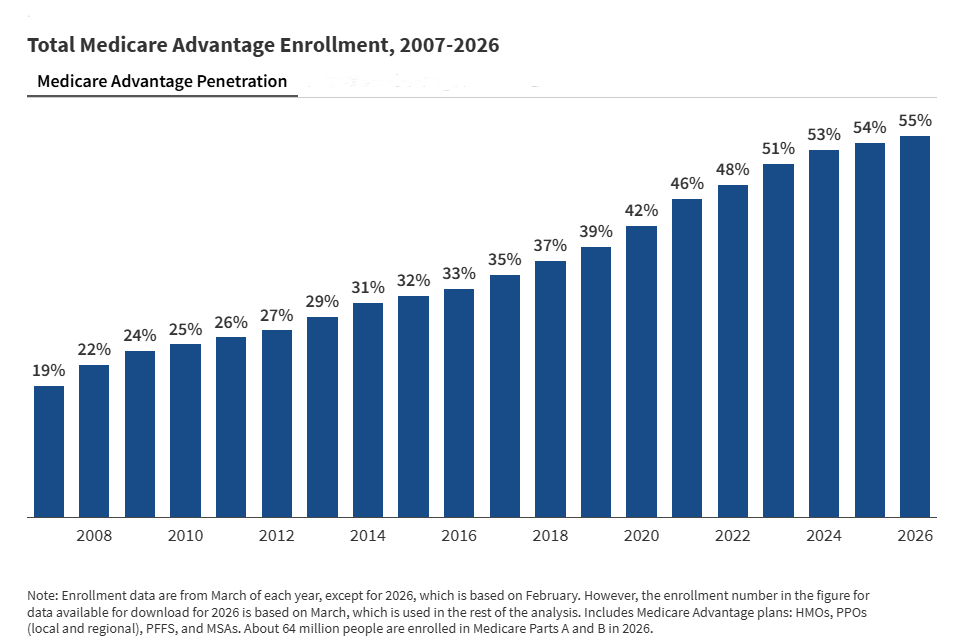
The Medicare Advantage plan was first introduced in 1997. As of 2025, KFF data shows more than half of eligible Medicare beneficiaries—or about 34.1 million people—are enrolled in plans. In January, the Centers for Medicare & Medicaid Services (CMS) released proposed rates for the 2027 plan year, which kept reimbursement rates essentially flat for the year.
Publisher: Source link