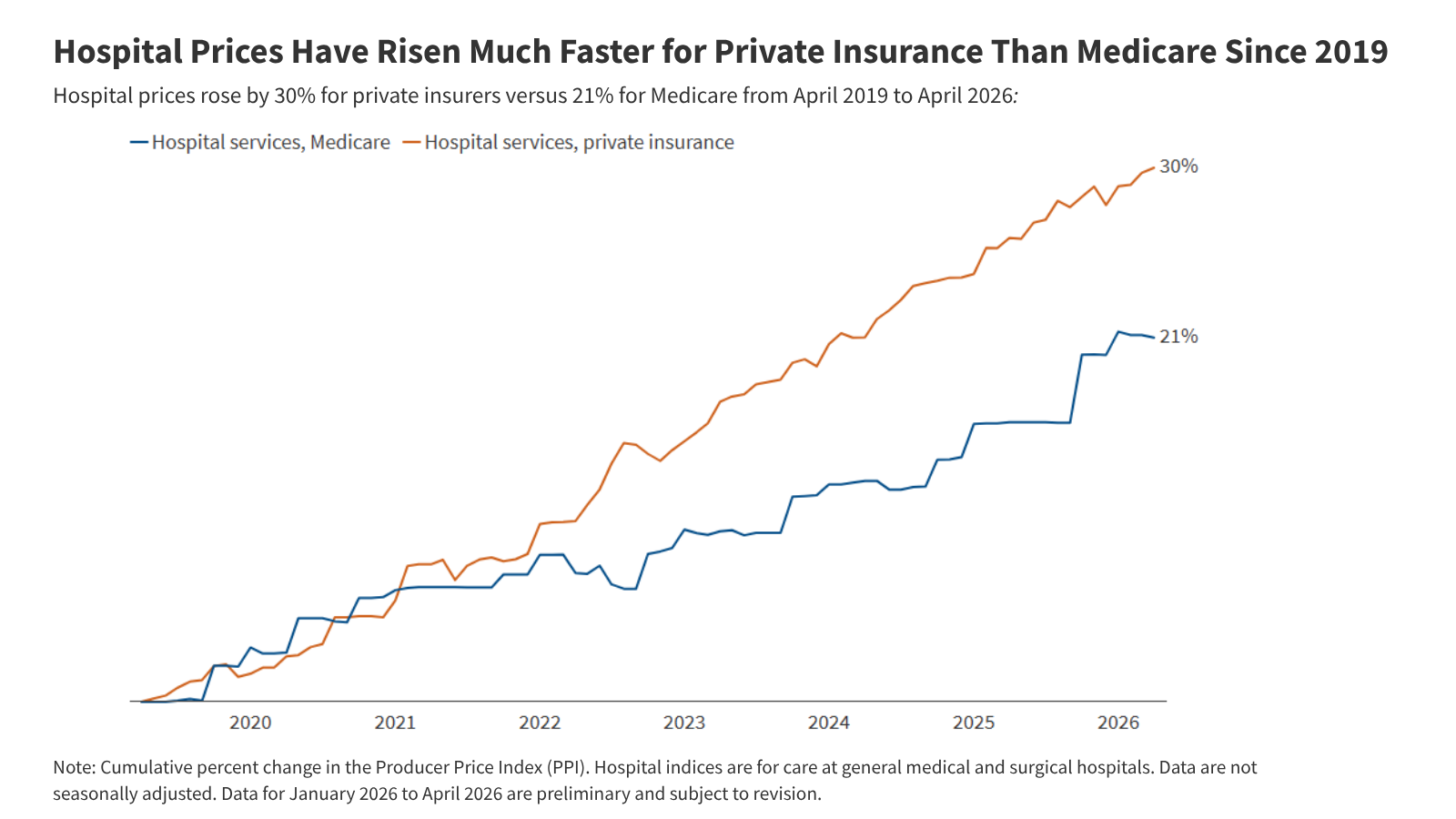
Private equity’s track record in healthcare could best be described as “mixed,” with high-profile failures like the implosion of Steward Health Care setting a poor example.
However, private investment will be even more critical for healthcare organizations in a political environment where public funds are likely to shrink. That’s why investors representing multiple sectors within the industry are collaborating with experts at the Duke-Margolis Institute for Health Policy to chart a better course forward.
This week, they announced the launch of the Duke-Margolis Capital Impact Council, which seeks to build the strategies and tools necessary to ensure that private equity partners are facilitating better health outcomes, access and affordability.
“Private investment, private equity, venture capital dollars really matter in healthcare,” said Cheryl Pegus, M.D., co-chair of the council and executive chair of Flyte Health, during a panel at the American College of Healthcare Executives’ Congress moderated by Fierce Healthcare.
“What we want to do is ensure that we’re looking at not just the financial value, but we’re also looking at what we call the health value, the impact on improving health outcomes,” she said.
Alongside Pegus, the council’s members include:
- David Brailer, The Cigna Group
- Craig Cimini, The Cigna Group Ventures
- Rob Coppedge, Echo Health Ventures
- Blake Goodner, Bridger Capital
- Gregory Grunberg, Temasek
- Marc Harrison, Health Assurance Transformation Corp.
- Dan Mendelson, Morgan Health
- Brian Morfitt, Frazier Healthcare Partners
- Amy B. Raimundo, KP Ventures
- Amir Dan Rubin, Healthier Capital
- Lee Shapiro, 7Wire
- Lisa Suennen, American Heart Association Ventures
Mark McClellan, M.D., director of the Margolis Center and former administrator of the Centers for Medicare & Medicaid Services, serves as Pegus’ fellow co-chair for the effort. Bob Margolis, founder of Duke-Margolis, and Marc Samuels, CEO of ADVI, are advisors for the council.
McClellan said that as the Trump administration and legislators on Capitol Hill put a focus on federal spending cuts, it will be even more imperative for private partners to fill in the gaps.
“This means to me that it’s a more important time than ever for the private sector to step up and show that it can deliver on supporting better, more innovative ways of delivering care,” he said during the panel.
The council’s first piece of work is a white paper released this week that highlights its “health value return on investment” (HV-ROI) framework. The guidelines establish metrics that can be used to track how well an organization is improving health alongside generating the expected financial ROI.
Elements to consider include the intended population, the impact on providers and the time until an investment bears fruit. Performance indicators within the framework range from clinical results, access, ease of use for providers, equity, community impact and more.
McClellan said that healthcare organizations are frequently bombarded with pitches and possibilities, and having a framework like this in place makes it easier to identify the most valuable opportunities.
“What we’re trying to do is bring some pressure, and I think in some ways, to relieve some pressure that’s out there among a lot of individual organizations that are trying to do something to get these areas to match up—the financial returns, the health value returns—but are having trouble just scaling that,” he said.
Alongside outlining the concept behind HV-ROI, the report highlights multiple case studies, or investments that the council’s members have made that are establishing an ROI around health outcomes.
For example, the American Heart Association Ventures backs Attane Health, which is a digital marketplace that connects patients with healthy foods, nutrition coaching and data with the goal of addressing food insecurity and related outcomes.
Within the HV-ROI framework, the team identified that there is a significant portion of the Medicaid population that faces food insecurity, and poor nutrition is a significant factor in multiple conditions such as diabetes and hypertension.
Attane has found that 70% of its users who have diabetes saw lowered blood pressure, and 90% of those who connected with its coaching services reported improvements to their health. These are key performance indicators that highlight the health value potential of Attane’s platform.
Pegus said that a critical element driving the council’s work forward is that she, McClellan and others on the council are approaching this topic through the lens of a physician, with the understanding of what they need to drive toward transformation and where the gaps may lie.
“We understand the clinical aspects of healthcare,” she said. “But if you’ve been doing this for a really long time, you’re really aware that when there is no funding, lots of things that you want to improve [in] healthcare just doesn’t happen.
“And so funding has to be not grant-related, not philanthropic,” Pegus said. “It has to be sustainable, and there has to be a way for us to measure that transparently so that we can continue to invest in healthcare.”
Publisher: Source link